
Obstructive sleep apnea syndrome (OSAS) is a collective term which also includes snoring and upper airway resistance syndrome (UARS). Simply put, the term is descriptive of the effects of a neurologic and anatomic partial collapse or total obstruction of the upper airway during sleep. The main effects are excessive daytime sleepiness (EDS), impaired cognition, and increased risk of motor vehicle accidents. The daytime sleepiness causes marked decrements in quality of life. Subjects with OSAS often have cardiovascular morbidities, hypertension, diabetes, myocardial infarction, stroke and sudden death. A shortened life span is common in subjects with untreated obstructive sleep apnea syndrome.
The nocturnal obstructive process in sleep disorders may be localized to one or two areas, or may encompass the entire upper airway passages.

This includes the nasal cavity, nasopharynx, oropharynx and hypopharynx. Conservative medical therapy is usually recommended first such as weight loss, exercise, sleep hygiene, dental appliances and continuous positive airway pressure (CPAP). Unfortunately, there is a significant compliance problem with medical devices used in the nasal region (CPAP).
There are surgical procedures presently available to provide for a logical upper airway reconstruction of these regions in such a manner as to minimize the risks and possible complications. A two-phased surgical protocol has been used to decrease the risk of over operating.
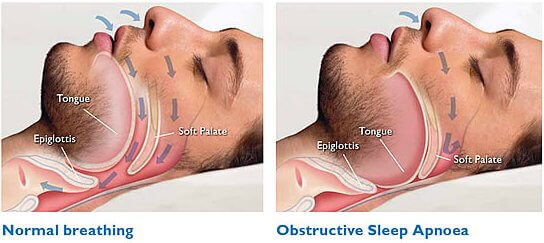
The most important part of the surgical work up for OSAS is to establish the potential for obstruction at each level of the upper airway (nose, palate, tonsils, and tongue base). A team approach including orthodontists and oral maxillo-facial surgeons determines the “best practice” for each individual patient.
Magnetic resonance imaging (MRI) is frequently used in sleep research. MRI scanning can be done asleep with a polysomnogram (PSG) and provides substantial data, but is lengthy and expensive. These three dimensional methods provide more information than traditional two dimensional (2D) radiographic imaging (Panorex and lateral Cephalometrics).
Fiberoptic endoscopy examinations can be performed awake or during drug-induced sleep endoscopy (DISE) using Propofol sedation. For drug-induced sleep endoscopy, the patient is under a general anesthetia. During sleep in patients with OSAS the airway narrows and starts to obstruct. Negative pressures are then generated which can further cause total airway obstruction. This process can be observed during sleep endoscopy.
Orthodontists and dentists have, for at least the last thirty years, focused on various methods of managing the anatomic pharyngeal airway for patients with OSAS. It is time to consider new methods for OSAS treatments, but with their own limitation in selected patients.
We cannot continue to think only in terms of the anatomic airway, as there are many theories for snoring and obstructive sleep apnea are available.
For instance, consider the possibility that turbulent “airflow” may cause nightly snoring and thus damage the delicate soft tissues of the upper airway. This may lead to group of symptoms:
So snoring is not a disorder but it may lead to many noninfected lifestyle disorders. If the person is suffering from above symptoms, just contact your ENT Surgeon Pulmonologist.
At the end, presence of above symptoms may not always indicate that the person is suffering from Obstructive sleep apnea disorder only. As it is told, “All that glitters are not gold But The Goldsmith can differentiate……“
Rains along with respite from scorching heat brings seasonal illnesses that deter people from enjoying the cool and pleasant atmosphere. Along with cold and flu, monsoon is a season of deadly diseases like Dengue, Chikungunya, Malaria, Typhoid, Cholera, Hepatitis A, etc. Monsoon...
Shalby Hospital in Ahmedabad has been providing top-notch medical services for more than three decades. We have gained a reputation for our expertise in eye and ear healthcare, making us the preferred choice for people looking for exceptional medical care in these...
Are you experiencing discomfort or pain in your ears, nose, or throat? If so, finding a reliable and skilled ENT specialist is crucial. Thankfully, Shalby Hospital is a reputable healthcare provider with a proven track record in the ear, nose, and throat...